Seeing blood after a bowel movement can be an alarming situation. While mainly caused by minor non-life-threatening conditions, it is still crucial to investigate to rule out more serious digestive diseases. Whether it appears on toilet paper after wiping, in the toilet bowl, or in stool, the specifics of the blood can offer clues to the cause and help determine when to seek more in-depth professional help.
This guide explains the most common causes of rectal bleeding, when to seek medical care, how doctors diagnose, and treatment options.
What Causes Rectal Bleeding?
Rectal bleeding – blood coming from the anus, rectum, or lower digestive tract – is commonly caused by a range of conditions like hemorrhoids, fissures, inflammation, and others. Seeing a doctor for any bleeding to be sure the issue is benign is of utmost importance.
Examining factors like color and frequency is important to note and share with your doctor. If blood is bright red, it usually points to an issue involving the anus and rectum. If blood is darker, it may indicate an issue higher in the digestive tract. Understanding how often and in what situations the bleeding occurs will also help your doctor better diagnose and provide treatment.
Below are the key causes for rectal bleeding, from most to least common.
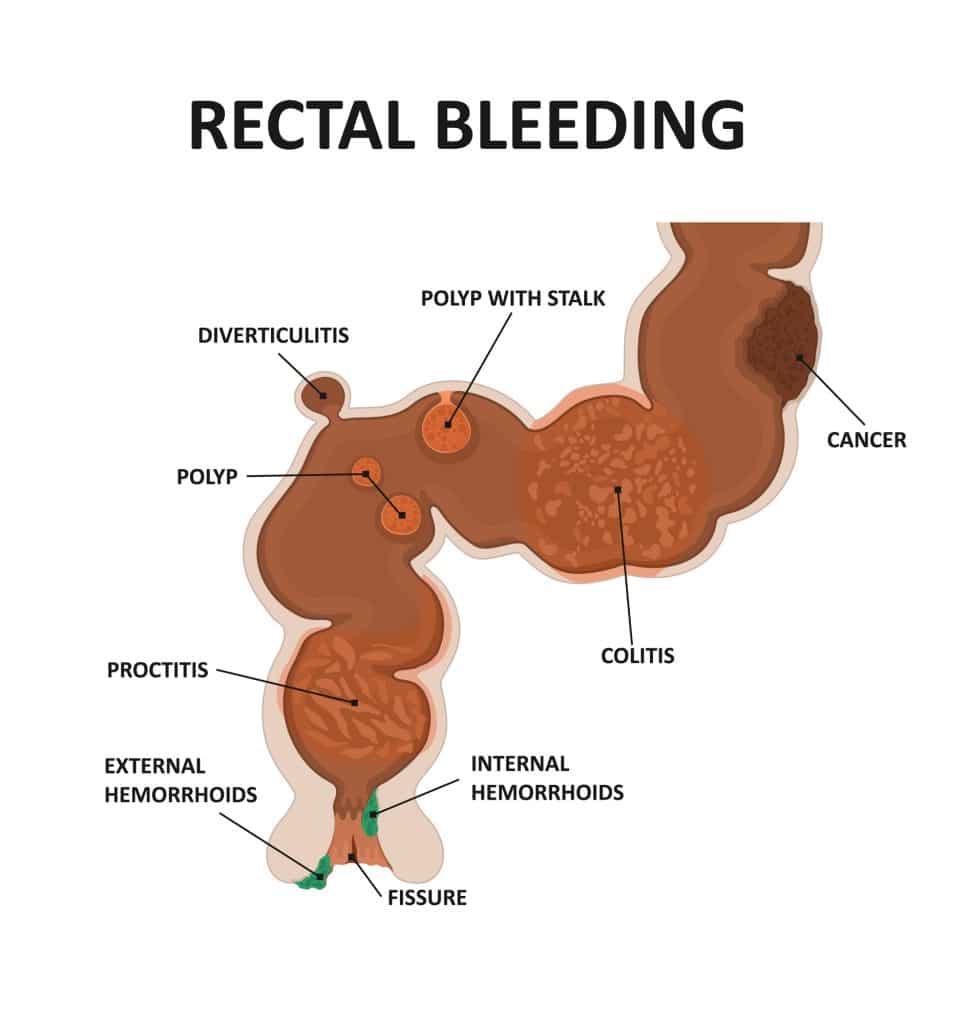
Hemorrhoids
Hemorrhoids are venous cushions located inside the anus and rectum. We have 6 hemorrhoids total, 3 internal and 3 external. External hemorrhoid veins live under the skin which is abundant in nerve endings, while internal hemorrhoid veins live under mucosa which lacks pain fibers. Most people don’t know they have hemorrhoids until they become symptomatic.
Hemorrhoids often develop due to:
- Straining during bowel movements
- Chronic constipation or diarrhea
- Prolonged sitting on the toilet
- Pregnancy
- Straining while lifting heavy objects
- Excessive coughing or sneezing
Although they are both venous cushions, internal and external hemorrhoids have completely different symptoms and treatment. When hemorrhoid veins become inflamed and enlarged, they can become symptomatic with swelling, bleeding pain, itching discomfort and urgency to defecate. Hemorrhoid bleeding is usually painless and mild but should still be evaluated if persistent.
R.H.O.I.D. is a natural supplement that can be taken for people who experience hemorrhoids.
Anal Fissures
An anal fissure is a small tear in the delicate lining of the anus that can occur due to hard stools, straining intensely during a bowel movement, diarrhea or trauma to the anal canal. It is similar to a paper cut on your finger or a split lip. Symptoms include:
- Sharp pain
- Bright red blood while wiping
- Burning or irritation
Fissures often heal on their own but may require treatment if chronic.
Diverticulitis
Diverticulitis is a condition where small pouches in the colon become inflamed and bleed. It is the most common cause of acute lower gastrointestinal bleeding in adults. The blood vessels around the pouches become weak and over time, the blood vessel lining ruptures, which leads to a large amount of bleeding. Medical evaluation is important to prevent complications.
Symptoms may include:
- Blood in stool
- Passing large volumes of fresh blood and/or clots
- An urgency to defecate
Polyps
Colon or rectal polyps are growths in the lining of the digestive tract. While many are benign, some can develop into cancer over time. It’s crucial to have routine colonoscopies if you are over 45 years old or if you experience any of the symptoms below to help detect and remove polyps early to prevent cancer. Symptoms may include:
- Blood in stool
- Bleeding while wiping
- Changes in bowel habits
- Abdominal pain
Proctitis
Proctitis is inflammation of the rectum lining that can be caused by inflammatory bowel disease, infections, or a side effect from radiation therapy.
Symptoms include:
- Rectal bleeding
- Pain in anus, rectum, or left abdomen
- Urgency to have bowel movements
Treatment is determined based on the underlying cause.
Anal Condyloma
Anal condyloma refers to genital warts caused by the human papillomavirus (HPV). These usually benign growths can develop around or inside the anus and may bleed when irritated.
Symptoms may include:
- Small growths near the anus
- Bleeding after wiping
- Itching or irritation
- Discomfort during bowel movements
Treatment typically involves topical medications or removal procedures.
Anal Cancer
The possibility of anal cancer is rare but serious. It may cause bleeding, pain, and changes in bowel habits. Rectal bleeding should never be assumed to be hemorrhoids without proper evaluation, since cancers can present similarly.
Symptoms may include:
- Persistent bleeding
- Anal pain or pressure
- Lump outside the anus
- Unexplained weight loss
Early diagnosis greatly improves treatment outcomes and you should never ignore symptoms.
When to Worry About Blood in Your Stool
While minor bleeding may resolve on its own, certain warning signs require prompt medical attention. Any bleeding, even if small and infrequent, should always be evaluated by a doctor to rule out any serious conditions. Colonoscopies are a crucial screening method to rule out polyps or cancer.
Other reasons to see a doctor include:
- Bleeding lasting more than a few days
- Heavy bleeding
- Black or tarry stool
- Passing clots of blood
- Unexplained weight loss
- Fever with bleeding
- Severe pain
- Changes in bowel habits

How to Find the Source of Rectal Bleeding
Doctors may use several methods to identify the cause of your rectal bleeding, including:
- Medical history review
- Physical examination
- Rectal exam
- Colonoscopy or endoscopy
Colonoscopies are one of the most effective tools for diagnosing the source of rectal bleeding and might be recommended after preliminary physical examination and lifestyle analysis.
How to Treat Rectal Bleeding
Treatment depends on the diagnosis of your rectal bleeding. Doctors often evaluate symptoms such as timing, stool appearance, and associated pain to determine the cause. Options may include:
Home Treatments
- Increasing fiber intake
- Drinking more water
- Avoiding straining
- Sitz baths
These methods may help some hemorrhoids and fissures heal but you should always seek the diagnosis and guidance of your doctor.
Office and Medical Treatments
- Office based therapies
- Injection sclerotherapy for internal hemorrhoids
- Rubber band ligation
- Infrared coagulation
- Prescription medications, antibiotics, or anti-inflammatory drugs
Surgical Treatments
In severe cases, different types of surgery may be necessary to remove polyps, treat hemorrhoids and chronic fissures, or address cancer.
When to See A Doctor for Anal Bleeding
While you might be reluctant to see a doctor about rectal bleeding, you should always seek medical counsel for any bleeding. Other more serious bleeding include:
- Bleeding persisting beyond a few days
- Bleeding recurring frequently
- Symptoms worsening with excessive bleeding or passing clots
Even if you are younger than 45, a colonoscopy could be warranted to rule out polyps or cancer. The key thing to remember is that rectal bleeding should never be ignored, even if mild.

What questions should I ask my doctor about rectal bleeding?
Questions to consider asking your doctor are:
- What do you think is causing my rectal bleeding?
- Do I need a colonoscopy?
- Could this be just hemorrhoids or something more serious?
- What at-home treatments are available?
- How can I prevent it from happening again?
Anal Bleeding FAQ
Can stress cause rectal bleeding?
Stress itself does not directly cause bleeding, but it can worsen digestive conditions such as hemorrhoids or inflammatory bowel disease, which may lead to bleeding. Stress also affects bowel movements – stress-induced constipation or diarrhea can lead to symptomatic hemorrhoid or anal fissure bleeding.
Is blood in your stool serious?
Blood in stool is serious because it points to an ailment that most of the time needs to be addressed. Any case of blood in your stool should be evaluated by a medical professional because it’s one of the cardinal signs of colorectal cancer. Anal bleeding from hemorrhoids or fissures can paint the outside of the stool with blood, while blood mixed in the stool is a more serious sign.
Is bright red blood in my stool worse than darker blood?
Not necessarily. Bright red blood usually comes from the lower digestive tract, while darker blood may originate higher up and could indicate different conditions. Blood of any shade requires medical evaluation.
Can straining too hard to poop cause rectal bleeding?
Yes, straining can cause hemorrhoids or anal fissures, both of which may lead to bleeding.
Final Thoughts on Rectal Bleeding
Seeing blood after pooping is common and often caused by hemorrhoids or fissures. However, it can also indicate more serious conditions. Any bleeding requires medical evaluation, especially for people younger than 45 or anyone who doesn’t get routine colonoscopies. Keep in mind, if you’ve had a recent colonoscopy, another one is not necessary.
Passing large volumes of blood or clots you should seek emergency care. Early diagnosis ensures proper treatment and peace of mind.
If you are experiencing blood on toilet paper after pooping, request an appointment with Dr. Rosenfeld today or call us at 805-230-2889 (BUTZ).

